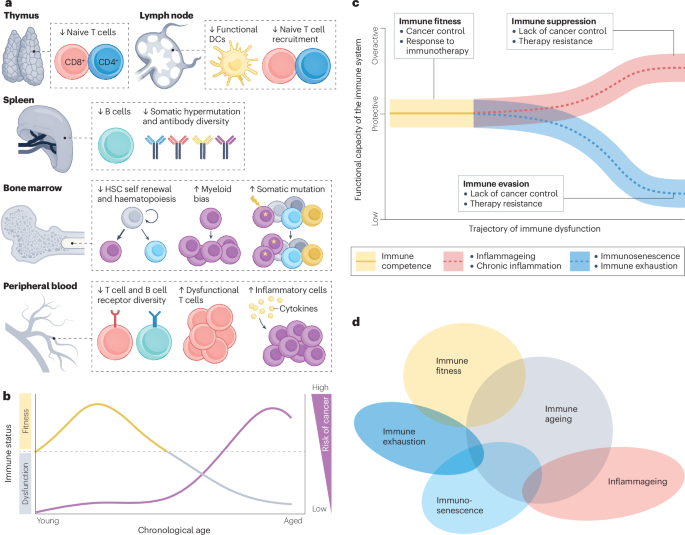
Ageing, immune fitness and cancer
Siegel, R. L., Giaquinto, A. N. & Jemal, A. Cancer statistics, 2024. CA Cancer J. Clin. 74, 12–49 (2024).
Google Scholar
Dorshkind, K., Montecino-Rodriguez, E. & Signer, R. A. J. The ageing immune system: is it ever too old to become young again? Nat. Rev. Immunol. 9, 57–62 (2009).
Google Scholar
Bray, F. et al. Global cancer statistics 2022: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 74, 229–263 (2024).
Google Scholar
VanderWalde, N. A. et al. Disparities in older adult accrual to cancer trials: analysis from the Alliance for Clinical Trials in Oncology (A151736). J. Geriatr. Oncol. 13, 20–26 (2022).
Google Scholar
Freedman, R. A. et al. Breast cancer-specific survival by age: worse outcomes for the oldest patients. Cancer 124, 2184–2191 (2018).
Google Scholar
Lancaster, J. N. Aging of lymphoid stromal architecture impacts immune responses. Semin. Immunol. 70, 101817 (2023).
Google Scholar
Han, S., Georgiev, P., Ringel, A. E., Sharpe, A. H. & Haigis, M. C. Age-associated remodeling of T cell immunity and metabolism. Cell Metab. 35, 36–55 (2023).
Google Scholar
Mogilenko, D. A., Shchukina, I. & Artyomov, M. N. Immune ageing at single-cell resolution. Nat. Rev. Immunol. 22, 484–498 (2022).
Google Scholar
Swanton, C. et al. Embracing cancer complexity: hallmarks of systemic disease. Cell 187, 1589–1616 (2024).
Google Scholar
Kalathoor, S. et al. Representation of women in clinical trials supporting FDA-approval of contemporary cancer therapies. Int. J. Cancer 155, 1958–1968 (2024).
Google Scholar
O’Rourke, K. New FDA guidance recommends increasing the number of older adults in cancer clinical trials: the guidance is intended to assist in evaluating cancer therapies in adults aged 65 years and older: the guidance is intended to assist in evaluating cancer therapies in adults aged 65 years and older. Cancer 128, 2397–2398 (2022).
Google Scholar
Lee, W., Wang, Z., Saffern, M., Jun, T. & Huang, K.-L. Genomic and molecular features distinguish young adult cancer from later-onset cancer. Cell Rep. 37, 110005 (2021).
Google Scholar
Zhou, A., Zhang, D., Kang, X. & Brooks, J. D. Identification of age- and immune-related gene signatures for clinical outcome prediction in lung adenocarcinoma. Cancer Med. 12, 17475–17490 (2023).
Google Scholar
Wu, Y. et al. Comprehensive transcriptome profiling in elderly cancer patients reveals aging-altered immune cells and immune checkpoints. Int. J. Cancer 144, 1657–1663 (2019).
Google Scholar
Erbe, R. et al. Evaluating the impact of age on immune checkpoint therapy biomarkers. Cell Rep. 36, 109599 (2021).
Google Scholar
Kugel, C. H. et al. Age correlates with response to anti-PD1, reflecting age-related differences in intratumoral effector and regulatory T-cell populations. Clin. Cancer Res. 24, 5347–5356 (2018).
Google Scholar
Chen, L., Zhang, M., Zhou, J., Zhang, L. & Liang, C. Establishment of an age- and tumor microenvironment-related gene signature for survival prediction in prostate cancer. Cancer Med. 11, 4374–4388 (2022).
Google Scholar
Shah, Y. et al. Pan-cancer analysis reveals molecular patterns associated with age. Cell Rep. 37, 110100 (2021).
Google Scholar
Park, M. D. et al. Hematopoietic aging promotes cancer by fueling IL-1α-driven emergency myelopoiesis. Science 386, eadn0327 (2024). This study shows how IL-1α alters haematopoietic stem and progenitor cells in the ageing bone marrow to facilitate myeloid cell production and immunosuppression in lung tumours.
Google Scholar
Qing, T. et al. Molecular differences between younger versus older ER-positive and HER2-negative breast cancers. NPJ Breast Cancer 8, 119 (2022).
Google Scholar
Takada, K. et al. Differences in tumor-infiltrating lymphocyte density and prognostic factors for breast cancer by patient age. World J. Surg. Oncol. 20, 38 (2022).
Google Scholar
Buja, A. et al. Cutaneous melanoma in older patients. BMC Geriatr. 24, 232 (2024).
Google Scholar
Brummel, K., Eerkens, A. L., de Bruyn, M. & Nijman, H. W. Tumour-infiltrating lymphocytes: from prognosis to treatment selection. Br. J. Cancer 128, 451–458 (2023).
Google Scholar
Jeske, S. S. et al. Age-related changes in T lymphocytes of patients with head and neck squamous cell carcinoma. Immun. Ageing 17, 3 (2020).
Google Scholar
Newman, A. M. et al. Robust enumeration of cell subsets from tissue expression profiles. Nat. Methods 12, 453–457 (2015).
Google Scholar
Yoshihara, K. et al. Inferring tumour purity and stromal and immune cell admixture from expression data. Nat. Commun. 4, 2612 (2013).
Google Scholar
Racle, J. & Gfeller, D. EPIC: a tool to estimate the proportions of different cell types from bulk gene expression data. Methods Mol. Biol. 2120, 233–248 (2020).
Google Scholar
Li, T. et al. TIMER: a web server for comprehensive analysis of tumor-infiltrating immune cells. Cancer Res. 77, e108–e110 (2017).
Google Scholar
Im, Y. & Kim, Y. A comprehensive overview of RNA deconvolution methods and their application. Mol. Cell 46, 99–105 (2023).
Google Scholar
Zhang, Z. et al. A panoramic view of cell population dynamics in mammalian aging. Science eadn3949, 387 (2025).
Tabula Muris Consortium. A single-cell transcriptomic atlas characterizes ageing tissues in the mouse. Nature 583, 590–595 (2020).
Mogilenko, D. A. et al. Comprehensive profiling of an aging immune system reveals clonal GZMK+ CD8+ T cells as conserved hallmark of inflammaging. Immunity 54, 99–115.e12 (2021). This study used a combination of scRNA-seq, TCR and B cell receptor analysis to assess the immune profile in multiple organs of aged mice and discovered a clonal GZMK+ CD8+ T cell population with pro-inflammatory activity that was also found in the circulation of older adults.
Google Scholar
Angarola, B. L. et al. Comprehensive single-cell aging atlas of healthy mammary tissues reveals shared epigenomic and transcriptomic signatures of aging and cancer. Nat. Aging 5, 122–143 (2024). This study demonstrated that distinct T cell subsets and macrophages expand in the aged mammary gland in mice and that transcriptional signatures of ageing mammary cells are enriched in human breast tumours.
Google Scholar
Tiberti, S. et al. GZMKhigh CD8+ T effector memory cells are associated with CD15high neutrophil abundance in non-metastatic colorectal tumors and predict poor clinical outcome. Nat. Commun. 13, 6752 (2022).
Google Scholar
Lan, F. et al. GZMK-expressing CD8+ T cells promote recurrent airway inflammatory diseases. Nature 638, 490–498 (2025).
Google Scholar
Wells, S. B. et al. Multimodal profiling reveals tissue-directed signatures of human immune cells altered with age. Preprint at bioRxiv (2024). This study uses CITE-seq to provide a comprehensive analysis of the human immune system across various tissues and donor ages, demonstrating that age-related changes in immune homeostasis are tissue specific.
Google Scholar
Wu, S. Z. et al. A single-cell and spatially resolved atlas of human breast cancers. Nat. Genet. 53, 1334–1347 (2021).
Google Scholar
Parsons, A. et al. Cell populations in human breast cancers are molecularly and biologically distinct with age. Preprint at Res. Sq. (2024). This is the first study to show subtype-specific age-related changes in the TIME of human breast cancer at single-cell resolution.
Google Scholar
Salcher, S. et al. High-resolution single-cell atlas reveals diversity and plasticity of tissue-resident neutrophils in non-small cell lung cancer. Cancer Cell 40, 1503–1520.e8 (2022).
Google Scholar
Safina, K. & van Galen, P. New frameworks for hematopoiesis derived from single-cell genomics. Blood 144, 1039–1047 (2024).
Google Scholar
Weisberg, S. P., Ural, B. B. & Farber, D. L. Tissue-specific immunity for a changing world. Cell 184, 1517–1529 (2021).
Google Scholar
McAllister, S. S. & Weinberg, R. A. The tumour-induced systemic environment as a critical regulator of cancer progression and metastasis. Nat. Cell Biol. 16, 717–727 (2014).
Google Scholar
Cao, R., Thatavarty, A. & King, K. Y. Forged in the fire: lasting impacts of inflammation on hematopoietic progenitors. Exp. Hematol. 134, 104215 (2024).
Google Scholar
Yang, D. & de Haan, G. Inflammation and aging of hematopoietic stem cells in their niche. Cells 10, 1849 (2021).
Google Scholar
Pietras, E. M. Inflammation: a key regulator of hematopoietic stem cell fate in health and disease. Blood 130, 1693–1698 (2017).
Google Scholar
Fotopoulou, F., Rodríguez-Correa, E., Dussiau, C. & Milsom, M. D. Reconsidering the usual suspects in age-related hematologic disorders: is stem cell dysfunction a root cause of aging? Exp. Hematol. 143, 104698 (2025).
Google Scholar
Kovtonyuk, L. V. et al. IL-1 mediates microbiome-induced inflammaging of hematopoietic stem cells in mice. Blood 139, 44–58 (2022).
Google Scholar
Caiado, F. & Manz, M. G. IL-1 in aging and pathologies of hematopoietic stem cells. Blood 144, 368–377 (2024).
Google Scholar
Jergović, M. et al. IL-6 can singlehandedly drive many features of frailty in mice. GeroScience 43, 539–549 (2021).
Google Scholar
Alvarez-Rodríguez, L., López-Hoyos, M., Muñoz-Cacho, P. & Martínez-Taboada, V. M. Aging is associated with circulating cytokine dysregulation. Cell. Immunol. 273, 124–132 (2012).
Google Scholar
Albani, D. et al. Interleukin-6 plasma level increases with age in an Italian elderly population (“The Treviso Longeva”-Trelong-study) with a sex-specific contribution of rs1800795 polymorphism. Age 31, 155–162 (2009).
Google Scholar
Beharka, A. A. et al. Interleukin-6 production does not increase with age. J. Gerontol. A Biol. Sci. Med. Sci. 56, B81–B88 (2001).
Google Scholar
Tylutka, A., Walas, Ł. & Zembron-Lacny, A. Level of IL-6, TNF, and IL-1β and age-related diseases: a systematic review and meta-analysis. Front. Immunol. 15, 1330386 (2024).
Google Scholar
Pietras, E. M. et al. Chronic interleukin-1 exposure drives haematopoietic stem cells towards precocious myeloid differentiation at the expense of self-renewal. Nat. Cell Biol. 18, 607–618 (2016).
Google Scholar
Chavez, J. S. et al. PU.1 enforces quiescence and limits hematopoietic stem cell expansion during inflammatory stress. J. Exp. Med. 218, e20201169 (2021).
Google Scholar
Frisch, B. J. et al. Aged marrow macrophages expand platelet-biased hematopoietic stem cells via Interleukin1B. JCI Insight 5, e124213 (2019).
Google Scholar
Ho, Y.-H. et al. Remodeling of bone marrow hematopoietic stem cell niches promotes myeloid cell expansion during premature or physiological aging. Cell Stem Cell 25, 407–418.e6 (2019).
Google Scholar
Zhao, J. L. et al. Conversion of danger signals into cytokine signals by hematopoietic stem and progenitor cells for regulation of stress-induced hematopoiesis. Cell Stem Cell 14, 445–459 (2014).
Google Scholar
Ridker, P. M. et al. Antiinflammatory therapy with canakinumab for atherosclerotic disease. N. Engl. J. Med. 377, 1119–1131 (2017).
Google Scholar
Ridker, P. M. et al. Effect of interleukin-1β inhibition with canakinumab on incident lung cancer in patients with atherosclerosis: exploratory results from a randomised, double-blind, placebo-controlled trial. Lancet 390, 1833–1842 (2017).
Google Scholar
Lythgoe, M. P. & Prasad, V. Repositioning canakinumab for non-small cell lung cancer-important lessons for drug repurposing in oncology. Br. J. Cancer 127, 785–787 (2022).
Google Scholar
US National Library of Medicine. ClinicalTrials.gov (2021).
Bruunsgaard, H., Skinhøj, P., Pedersen, A. N., Schroll, M. & Pedersen, B. K. Ageing, tumour necrosis factor-alpha (TNF-α) and atherosclerosis. Clin. Exp. Immunol. 121, 255–260 (2000).
Google Scholar
SanMiguel, J. M. et al. Distinct tumor necrosis factor alpha receptors dictate stem cell fitness versus lineage output in Dnmt3a-mutant clonal hematopoiesis. Cancer Discov. 12, 2763–2773 (2022). This study decouples the fitness and lineage bias effects of age-associated TNF signalling in DNMT3A-mutant clonal haematopoiesis.
Google Scholar
Liu, Z. G. Molecular mechanism of TNF signaling and beyond. Cell Res. 15, 24–27 (2005).
Google Scholar
Yamashita, M. & Passegué, E. TNF-α coordinates hematopoietic stem cell survival and myeloid regeneration. Cell Stem Cell 25, 357–372.e7 (2019).
Google Scholar
He, H. et al. Aging-induced IL27Ra signaling impairs hematopoietic stem cells. Blood 136, 183–198 (2020).
Google Scholar
Jakobsen, N. A. et al. Selective advantage of mutant stem cells in human clonal hematopoiesis is associated with attenuated response to inflammation and aging. Cell Stem Cell 31, 1127–1144.e17 (2024). Although bone marrow HSCs from individuals with CHIP show increased inflammatory gene expression compared with individuals without CHIP, within the CHIP marrow, DNMT3A-mutant and TET2-mutant HSCs have attenuated inflammatory signalling compared with wild-type HSCs.
Google Scholar
Cheong, J.-G. et al. Epigenetic memory of coronavirus infection in innate immune cells and their progenitors. Cell 186, 3882–3902.e24 (2023).
Google Scholar
Zeng, A. G. X. et al. Identification of a human hematopoietic stem cell subset that retains memory of inflammatory stress. Preprint at bioRxiv (2023). This study shows the presence of multiple HSC subsets in humans, including an inflammatory memory HSC subset induced by inflammatory stress stimuli.
Google Scholar
Kain, B. N. et al. Hematopoietic stem and progenitor cells confer cross-protective trained immunity in mouse models. iScience 26, 107596 (2023). This study establishes that inflammatory memory can be encoded at the stem cell level using transplantation of highly purified inflammation-exposed mouse HSCs.
Google Scholar
Mills, T. S. et al. A distinct metabolic and epigenetic state drives trained immunity in HSC-derived macrophages from autoimmune mice. Cell Stem Cell 31, 1630–1649.e8 (2024).
Google Scholar
Shiozawa, S. et al. Age distribution of circulating alpha-interferon. Experientia 45, 764–765 (1989).
Google Scholar
Helbling, P. M. et al. Global transcriptomic profiling of the bone marrow stromal microenvironment during postnatal development, aging, and inflammation. Cell Rep. 29, 3313–3330.e4 (2019).
Google Scholar
Benayoun, B. A. et al. Remodeling of epigenome and transcriptome landscapes with aging in mice reveals widespread induction of inflammatory responses. Genome Res. 29, 697–709 (2019).
Google Scholar
Havas, A. P. et al. Activated interferon signaling suppresses age-dependent liver cancer. Preprint at bioRxiv (2024).
Google Scholar
Baldridge, M. T., King, K. Y., Boles, N. C., Weksberg, D. C. & Goodell, M. A. Quiescent haematopoietic stem cells are activated by IFN-γ in response to chronic infection. Nature 465, 793–797 (2010).
Google Scholar
Essers, M. A. G. et al. IFNα activates dormant haematopoietic stem cells in vivo. Nature 458, 904–908 (2009).
Google Scholar
Bogeska, R. et al. Inflammatory exposure drives long-lived impairment of hematopoietic stem cell self-renewal activity and accelerated aging. Cell Stem Cell 29, 1273–1284.e8 (2022).
Google Scholar
Kristinsson, S. Y. et al. Chronic immune stimulation might act as a trigger for the development of acute myeloid leukemia or myelodysplastic syndromes. J. Clin. Oncol. 29, 2897–2903 (2011). This longitudinal population study links a history of infections or autoimmune diseases to an increased risk of myelodysplastic syndromes and acute myeloid leukaemia.
Google Scholar
Rönkkö, R. M., Nevala, A. O., Pitkäniemi, J. M., Wartiovaara-Kautto, U. M. & Malila, N. K. Subsequent malignant neoplasms after primary hematological malignancy in adult patients. Int. J. Cancer 155, 1007–1013 (2024).
Google Scholar
Lenz, A., Franklin, G. A. & Cheadle, W. G. Systemic inflammation after trauma. Injury 38, 1336–1345 (2007).
Google Scholar
Eskesen, T. O. et al. Association of trauma with long-term risk of death and immune-mediated or cancer disease in same-sex twins. JAMA Surg. 158, 738–745 (2023).
Google Scholar
Mitchell, E. et al. Clonal dynamics of haematopoiesis across the human lifespan. Nature 606, 343–350 (2022).
Google Scholar
Weng, C. et al. Deciphering cell states and genealogies of human haematopoiesis. Nature 627, 389–398 (2024). This study used multimodal single-cell analysis to quantify HSC clones and their output from human bone marrow samples.
Google Scholar
Razavi, P. et al. High-intensity sequencing reveals the sources of plasma circulating cell-free DNA variants. Nat. Med. 25, 1928–1937 (2019).
Google Scholar
Young, A. L., Challen, G. A., Birmann, B. M. & Druley, T. E. Clonal haematopoiesis harbouring AML-associated mutations is ubiquitous in healthy adults. Nat. Commun. 7, 12484 (2016).
Google Scholar
Belizaire, R., Wong, W. J., Robinette, M. L. & Ebert, B. L. Clonal haematopoiesis and dysregulation of the immune system. Nat. Rev. Immunol. 23, 595–610 (2023).
Google Scholar
Caiado, F. et al. Aging drives Tet2+/− clonal hematopoiesis via IL-1 signaling. Blood 141, 886–903 (2023).
Google Scholar
Quin, C. et al. Chronic TNF in the aging microenvironment exacerbates Tet2 loss-of-function myeloid expansion. Blood Adv. 8, 4169–4180 (2024).
Google Scholar
Zioni, N. et al. Inflammatory signals from fatty bone marrow support DNMT3A driven clonal hematopoiesis. Nat. Commun. 14, 2070 (2023).
Google Scholar
Liao, M. et al. Aging-elevated inflammation promotes DNMT3A R878H-driven clonal hematopoiesis. Acta Pharm. Sin. B. 12, 678–691 (2022).
Google Scholar
Heimlich, J. B. et al. Multiomic profiling of human clonal hematopoiesis reveals genotype and cell-specific inflammatory pathway activation. Blood Adv. 8, 3665–3678 (2024).
Google Scholar
Arends, C. M. et al. Hematopoietic lineage distribution and evolutionary dynamics of clonal hematopoiesis. Leukemia 32, 1908–1919 (2018).
Google Scholar
Buscarlet, M. et al. Lineage restriction analyses in CHIP indicate myeloid bias for TET2 and multipotent stem cell origin for DNMT3A. Blood 132, 277–280 (2018).
Google Scholar
Kasbekar, M., Mitchell, C. A., Proven, M. A. & Passegué, E. Hematopoietic stem cells through the ages: a lifetime of adaptation to organismal demands. Cell Stem Cell 30, 1403–1420 (2023).
Google Scholar
Colom Díaz, P. A., Mistry, J. J. & Trowbridge, J. J. Hematopoietic stem cell aging and leukemia transformation. Blood 142, 533–542 (2023).
Google Scholar
Yamamoto, R. et al. Large-scale clonal analysis resolves aging of the mouse hematopoietic stem cell compartment. Cell Stem Cell 22, 600–607.e4 (2018).
Google Scholar
Young, K. et al. Decline in IGF1 in the bone marrow microenvironment initiates hematopoietic stem cell aging. Cell Stem Cell 28, 1473–1482.e7 (2021).
Google Scholar
Nishi, K. et al. Alteration of long and short-term hematopoietic stem cell ratio causes myeloid-biased hematopoiesis. eLife (2025).
Tharmapalan, V. & Wagner, W. Biomarkers for aging of blood — how transferable are they between mice and humans? Exp. Hematol. 140, 104600 (2024).
Google Scholar
Kuranda, K. et al. Age-related changes in human hematopoietic stem/progenitor cells. Aging Cell 10, 542–546 (2011).
Google Scholar
Amoah, A. et al. Aging of human hematopoietic stem cells is linked to changes in Cdc42 activity. Haematologica 107, 393–402 (2022).
Google Scholar
Pang, W. W. et al. Human bone marrow hematopoietic stem cells are increased in frequency and myeloid-biased with age. Proc. Natl Acad. Sci. USA 108, 20012–20017 (2011).
Google Scholar
Alpert, A. et al. A clinically meaningful metric of immune age derived from high-dimensional longitudinal monitoring. Nat. Med. 25, 487–495 (2019). This study was the first to leverage immune-omics population data in a longitudinal framework to develop an immune ageing score, IMM-AGE, which is distinct from chronological age and predicts all-cause mortality, outperforming other established risk assessment algorithms.
Google Scholar
Chang, S.-T. et al. Age-dependent immune profile in healthy individuals: an original study, systematic review and meta-analysis. Immun. Ageing 21, 75 (2024).
Google Scholar
Huang, Z. et al. Effects of sex and aging on the immune cell landscape as assessed by single-cell transcriptomic analysis. Proc. Natl Acad. Sci. USA 118, e2023216118 (2021).
Google Scholar
Burel, J. G. et al. An integrated workflow to assess technical and biological variability of cell population frequencies in human peripheral blood by flow cytometry. J. Immunol. 198, 1748–1758 (2017).
Google Scholar
Márquez, E. J. et al. Sexual-dimorphism in human immune system aging. Nat. Commun. 11, 751 (2020).
Google Scholar
Luo, O. J. et al. Multidimensional single-cell analysis of human peripheral blood reveals characteristic features of the immune system landscape in aging and frailty. Nat. Aging 2, 348–364 (2022).
Google Scholar
Filippov, I., Schauser, L. & Peterson, P. An integrated single-cell atlas of blood immune cells in aging. NPJ Aging 10, 59 (2024).
Google Scholar
Furer, N. et al. A reference model of circulating hematopoietic stem cells across the lifespan with applications to diagnostics. Nat. Med. 31, 2442–2451 (2025).
Google Scholar
van Bergen, M. G. J. M. et al. Clonal hematopoiesis and myeloid skewing in older population-based individuals. Am. J. Hematol. 99, 2402–2405 (2024).
Google Scholar
Eller, L. A. et al. Reference intervals in healthy adult Ugandan blood donors and their impact on conducting international vaccine trials. PLoS One 3, e3919 (2008).
Google Scholar
Peng, L. et al. Effects of biological variations on platelet count in healthy subjects in China. Thromb. Haemost. 91, 367–372 (2004).
Google Scholar
Cohen, N. M. et al. Personalized lab test models to quantify disease potentials in healthy individuals. Nat. Med. 27, 1582–1591 (2021). This study takes an original approach to predict disease by large-scale mining of laboratory tests from electronic health record data mining.
Google Scholar
Mittelbrunn, M. & Kroemer, G. Hallmarks of T cell aging. Nat. Immunol. 22, 687–698 (2021).
Google Scholar
Britanova, O. V. et al. Age-related decrease in TCR repertoire diversity measured with deep and normalized sequence profiling. J. Immunol. 192, 2689–2698 (2014).
Google Scholar
Nikolich-Zugich, J. Ageing and life-long maintenance of T-cell subsets in the face of latent persistent infections. Nat. Rev. Immunol. 8, 512–522 (2008).
Google Scholar
Yager, E. J. et al. Age-associated decline in T cell repertoire diversity leads to holes in the repertoire and impaired immunity to influenza virus. J. Exp. Med. 205, 711–723 (2008).
Google Scholar
Cicin-Sain, L. et al. Loss of naive T cells and repertoire constriction predict poor response to vaccination in old primates. J. Immunol. 184, 6739–6745 (2010).
Google Scholar
Adeegbe, D., Matsutani, T., Yang, J., Altman, N. H. & Malek, T. R. CD4+ CD25+ Foxp3+ T regulatory cells with limited TCR diversity in control of autoimmunity. J. Immunol. 184, 56–66 (2010).
Google Scholar
Lorenzi, A. R. et al. Determination of thymic function directly from peripheral blood: a validated modification to an established method. J. Immunol. Methods 339, 185–194 (2008).
Google Scholar
Nishida, J. et al. Peripheral blood TCR clonotype diversity as an age-associated marker of breast cancer progression. Proc. Natl Acad. Sci. USA 120, e2316763120 (2023).
Google Scholar
Manuel, M. et al. Lymphopenia combined with low TCR diversity (divpenia) predicts poor overall survival in metastatic breast cancer patients. Oncoimmunology 1, 432–440 (2012).
Google Scholar
Luo, W. et al. Normalization of T cell receptor repertoire diversity in patients with advanced colorectal cancer who responded to chemotherapy. Cancer Sci. 102, 706–712 (2011).
Google Scholar
Salih, Z. et al. T cell immune awakening in response to immunotherapy is age-dependent. Eur. J. Cancer 162, 11–21 (2022).
Google Scholar
McAllister, S. S. et al. Systemic endocrine instigation of indolent tumor growth requires osteopontin. Cell 133, 994–1005 (2008).
Google Scholar
Direkze, N. C. et al. Bone marrow contribution to tumor-associated myofibroblasts and fibroblasts. Cancer Res. 64, 8492–8495 (2004).
Google Scholar
Worthley, D. L. et al. Human gastrointestinal neoplasia-associated myofibroblasts can develop from bone marrow-derived cells following allogeneic stem cell transplantation. Stem Cell 27, 1463–1468 (2009).
Google Scholar
Miller, T. E. et al. Mitochondrial variant enrichment from high-throughput single-cell RNA sequencing resolves clonal populations. Nat. Biotechnol. 40, 1030–1034 (2022).
Google Scholar
Miller, T. E. et al. Programs, origins, and niches of immunomodulatory myeloid cells in gliomas. Nature 640, 1072–1082 (2025).
Google Scholar
Shlush, L. I. et al. Identification of pre-leukaemic haematopoietic stem cells in acute leukaemia. Nature 506, 328–333 (2014).
Google Scholar
Severson, E. A. et al. Detection of clonal hematopoiesis of indeterminate potential in clinical sequencing of solid tumor specimens. Blood 131, 2501–2505 (2018).
Google Scholar
Swisher, E. M. et al. Somatic mosaic mutations in PPM1D and TP53 in the blood of women with ovarian carcinoma. JAMA Oncol. 2, 370–372 (2016).
Google Scholar
Coombs, C. C. et al. Identification of clonal hematopoiesis mutations in solid tumor patients undergoing unpaired next-generation sequencing assays. Clin. Cancer Res. 24, 5918–5924 (2018).
Google Scholar
Zajkowicz, A. et al. Truncating mutations of PPM1D are found in blood DNA samples of lung cancer patients. Br. J. Cancer 112, 1114–1120 (2015).
Google Scholar
Mayerhofer, C. et al. Clonal hematopoiesis in older patients with breast cancer receiving chemotherapy. J. Natl Cancer Inst. 115, 981–988 (2023).
Google Scholar
Ptashkin, R. N. et al. Prevalence of clonal hematopoiesis mutations in tumor-only clinical genomic profiling of solid tumors. JAMA Oncol. 4, 1589–1593 (2018).
Google Scholar
Comen, E. A. et al. Evaluating clonal hematopoiesis in tumor-infiltrating leukocytes in breast cancer and secondary hematologic malignancies. J. Natl Cancer Inst. 112, 107–110 (2020).
Google Scholar
Bolton, K. L. et al. Managing clonal hematopoiesis in patients with solid tumors. J. Clin. Oncol. 37, 7–11 (2019).
Google Scholar
Coombs, C. C. et al. Therapy-related clonal hematopoiesis in patients with non-hematologic cancers is common and associated with adverse clinical outcomes. Cell Stem Cell 21, 374–382.e4 (2017).
Google Scholar
Kleppe, M. et al. Somatic mutations in leukocytes infiltrating primary breast cancers. NPJ Breast Cancer 1, 15005 (2015).
Google Scholar
Marchetti, A. et al. Impact of clonal hematopoiesis of indeterminate potential on hepatocellular carcinoma in individuals with steatotic liver disease. Hepatology 80, 816–827 (2024).
Google Scholar
Buttigieg, M. M., Vlasschaert, C., Bick, A. G., Vanner, R. J. & Rauh, M. J. Inflammatory reprogramming of the solid tumor microenvironment by infiltrating clonal hematopoiesis is associated with adverse outcomes. Cell Rep. Med. 6, 101989 (2025).
Google Scholar
Pich, O. et al. Tumor-infiltrating clonal hematopoiesis. N. Engl. J. Med. 392, 1594–1608 (2025). This study shows that the presence of TI-CH in patients with NSCLC associates with increased recurrence and demonstrates that TI-CH can remodel the TIME and promote tumour organoid growth in mice.
Google Scholar
Feng, Y. et al. Hematopoietic-specific heterozygous loss of Dnmt3a exacerbates colitis-associated colon cancer. J. Exp. Med. 220, e20230011 (2023). This is the first demonstration of a causal relationship between a CHIP mutation in HSCs and the progression of a solid tumour.
Google Scholar
McAllister, S. S. & Weinberg, R. A. Tumor-host interactions: a far-reaching relationship. J. Clin. Oncol. 28, 4022–4028 (2010).
Google Scholar
Redig, A. J. & McAllister, S. S. Breast cancer as a systemic disease: a view of metastasis. J. Intern. Med. 274, 113–126 (2013).
Google Scholar
Elkabets, M. et al. Human tumors instigate granulin-expressing hematopoietic cells that promote malignancy by activating stromal fibroblasts in mice. J. Clin. Invest. 121, 784–799 (2011).
Google Scholar
Medrek, C., Pontén, F., Jirström, K. & Leandersson, K. The presence of tumor associated macrophages in tumor stroma as a prognostic marker for breast cancer patients. BMC Cancer 12, 306 (2012).
Google Scholar
Bateman, A., Cheung, S. T. & Bennett, H. P. J. A brief overview of progranulin in health and disease. Methods Mol. Biol. 1806, 3–15 (2018).
Google Scholar
Marsh, T. et al. Hematopoietic age at onset of triple-negative breast cancer dictates disease aggressiveness and progression. Cancer Res. 76, 2932–2943 (2016). This study was the first to demonstrate that age alters the haematopoiesis–cancer axis, showing that bone marrow-derived haematopoietic cells from young mice promote TNBC progression by supporting a tumour-supportive microenvironment, while ageing diminishes their pro-tumorigenic capacity.
Google Scholar
Mitchell, C. A. et al. Stromal niche inflammation mediated by IL-1 signalling is a targetable driver of haematopoietic ageing. Nat. Cell Biol. 25, 30–41 (2023).
Google Scholar
Ho, T. T. et al. Aged hematopoietic stem cells are refractory to bloodborne systemic rejuvenation interventions. J. Exp. Med. 218, e20210223 (2021).
Google Scholar
Ramalingam, P. et al. Restoring bone marrow niche function rejuvenates aged hematopoietic stem cells by reactivating the DNA damage response. Nat. Commun. 14, 2018 (2023).
Google Scholar
Dellorusso, P. V. et al. Autophagy counters inflammation-driven glycolytic impairment in aging hematopoietic stem cells. Cell Stem Cell 31, 1020–1037.e9 (2024).
Google Scholar
Ross, J. B. et al. Depleting myeloid-biased haematopoietic stem cells rejuvenates aged immunity. Nature 628, 162–170 (2024).
Google Scholar
Wang, Y. et al. Reducing functionally defective old HSCs alleviates aging-related phenotypes in old recipient mice. Cell Res. 35, 45–58 (2025).
Google Scholar
Wang, S., Lai, X., Deng, Y. & Song, Y. Correlation between mouse age and human age in anti-tumor research: significance and method establishment. Life Sci. 242, 117242 (2020).
Google Scholar
Anczuków, O. et al. Challenges and opportunities for modeling aging and cancer. Cancer Cell 41, 641–645 (2023).
Google Scholar
Yuan, R. et al. Aging in inbred strains of mice: study design and interim report on median lifespans and circulating IGF1 levels. Aging Cell 8, 277–287 (2009).
Google Scholar
Brayton, C. F., Treuting, P. M. & Ward, J. M. Pathobiology of aging mice and GEM: background strains and experimental design. Vet. Pathol. 49, 85–105 (2012).
Google Scholar
Hale, J. S., Boursalian, T. E., Turk, G. L. & Fink, P. J. Thymic output in aged mice. Proc. Natl Acad. Sci. USA 103, 8447–8452 (2006).
Google Scholar
Sceneay, J. et al. Interferon signaling is diminished with age and is associated with immune checkpoint blockade efficacy in triple-negative breast cancer. Cancer Discov. 9, 1208–1227 (2019). This study demonstrated that aged-related immune dysfunction limits immune-checkpoint blockade efficacy in TNBC, with parallel deficits observed in both aged mice and older patients with TNBC, highlighting age as a critical determinant of ICI responses.
Google Scholar
Zhivaki, D. et al. Correction of age-associated defects in dendritic cells enables CD4+ T cells to eradicate tumors. Cell 187, 3888–3903.e18 (2024). This study demonstrated that hyperactivating DCs using a vaccine adjuvant overcomes ageing-related deficiencies in antitumour immunity by improving DC migration and induction of cytotoxic TH1 CD4+ T cells in aged mice.
Google Scholar
Chen, A. C. Y. et al. The aged tumor microenvironment limits T cell control of cancer. Nat. Immunol. 25, 1033–1045 (2024). This study used scRNAseq to reveal an age-associated dysfunctional CD8+ T cell subset that promotes tumour progression in aged mice, and showed that impaired NK–DC–CD8+ T cell crosstalk can be restored by myeloid cell activation using a CD40 agonist.
Google Scholar
Georgiev, P. et al. Age-associated contraction of tumor-specific T cells impairs antitumor immunity. Cancer Immunol. Res. 12, 1525–1541 (2024). This study established that aged mice have fewer tumour antigen-specific CD8+ T cells and that transferring antigen-specific CD8+ T cells from young mice to aged mice could improve PD1-checkpoint blockade efficacy.
Google Scholar
Sitnikova, S. I. et al. Age-induced changes in anti-tumor immunity alter the tumor immune infiltrate and impact response to immuno-oncology treatments. Front. Immunol. 14, 1258291 (2023).
Google Scholar
Norian, L. A. & Allen, P. M. No intrinsic deficiencies in CD8+ T cell-mediated antitumor immunity with aging. J. Immunol. 173, 835–844 (2004).
Google Scholar
Lee-Chang, C. et al. Accumulation of 4-1BBL+ B cells in the elderly induces the generation of granzyme-B+ CD8+ T cells with potential antitumor activity. Blood 124, 1450–1459 (2014).
Google Scholar
Zhang, C. et al. Single-cell sequencing reveals antitumor characteristics of intratumoral immune cells in old mice. J. Immunother. Cancer 9, e002809 (2021).
Google Scholar
Duong, L. et al. Macrophage depletion in elderly mice improves response to tumor immunotherapy, increases anti-tumor T cell activity and reduces treatment-induced cachexia. Front. Genet. 9, 526 (2018).
Google Scholar
Oh, J., Magnuson, A., Benoist, C., Pittet, M. J. & Weissleder, R. Age-related tumor growth in mice is related to integrin α4 in CD8+ T cells. JCI Insight 3, e122961 (2018).
Google Scholar
Henry, C. J. & DeGregori, J. Modelling the ageing dependence of cancer evolutionary trajectories. Nat. Rev. Cancer (2025).
Google Scholar
Mellman, I., Chen, D. S., Powles, T. & Turley, S. J. The cancer-immunity cycle: indication, genotype, and immunotype. Immunity 56, 2188–2205 (2023). This publication updates the foundational cancer-immunity cycle framework, emphasizing the growing complexity of tumour–immune interactions, the dual roles of various immune cell types in promoting or suppressing antitumour responses, and the relevance of categorizing tumours by their immunological phenotype, or ‘immunotype’.
Google Scholar
Grizzle, W. E. et al. Age-related increase of tumor susceptibility is associated with myeloid-derived suppressor cell mediated suppression of T cell cytotoxicity in recombinant inbred BXD12 mice. Mech. Ageing Dev. 128, 672–680 (2007).
Google Scholar
Kallies, A. & Good-Jacobson, K. L. Transcription factor T-bet orchestrates lineage development and function in the immune system. Trends Immunol. 38, 287–297 (2017).
Google Scholar
Tsukamoto, H., Senju, S., Matsumura, K., Swain, S. L. & Nishimura, Y. IL-6-mediated environmental conditioning of defective Th1 differentiation dampens antitumour immune responses in old age. Nat. Commun. 6, 6702 (2015). This study demonstrated that elevated IL-6 impairs CD4+ T cell differentiation and CD8+ T cell-mediated tumour control in aged mice.
Google Scholar
Jagger, A., Shimojima, Y., Goronzy, J. J. & Weyand, C. M. Regulatory T cells and the immune aging process: a mini-review. Gerontology 60, 130–137 (2014).
Google Scholar
Elyahu, Y. et al. Aging promotes reorganization of the CD4 T cell landscape toward extreme regulatory and effector phenotypes. Sci. Adv. 5, eaaw8330 (2019).
Google Scholar
Okła, K., Farber, D. L. & Zou, W. Tissue-resident memory T cells in tumor immunity and immunotherapy. J. Exp. Med. 218, e20201605 (2021).
Google Scholar
Malik, B. T. et al. Resident memory T cells in the skin mediate durable immunity to melanoma. Sci. Immunol. 2, eaam6346 (2017).
Google Scholar
Gavil, N. V., Cheng, K. & Masopust, D. Resident memory T cells and cancer. Immunity 57, 1734–1751 (2024).
Google Scholar
Luoma, A. M. et al. Tissue-resident memory and circulating T cells are early responders to pre-surgical cancer immunotherapy. Cell 185, 2918–2935.e29 (2022).
Google Scholar
Pei, S. et al. Age-related decline in CD8+ tissue resident memory T cells compromises antitumor immunity. Nat. Aging 4, 1828–1844 (2024). This study showed reduced CD8+ TRM cells in the lung and liver of aged mice, leading to impaired antitumour immune control.
Google Scholar
Schenkel, J. M. & Masopust, D. Tissue-resident memory T cells. Immunity 41, 886–897 (2014).
Google Scholar
Pei, S. et al. BFAR coordinates TGFβ signaling to modulate Th9-mediated cancer immunotherapy. J. Exp. Med. 218, e20202144 (2021).
Google Scholar
du Halgouet, A. et al. Multimodal profiling reveals site-specific adaptation and tissue residency hallmarks of γδ T cells across organs in mice. Nat. Immunol. 25, 343–356 (2024).
Google Scholar
Thome, J. J. C. et al. Spatial map of human T cell compartmentalization and maintenance over decades of life. Cell 159, 814–828 (2014).
Google Scholar
de Mol, J., Kuiper, J., Tsiantoulas, D. & Foks, A. C. The dynamics of B cell aging in health and disease. Front. Immunol. 12, 733566 (2021).
Google Scholar
Zhang, E. et al. Roles and mechanisms of tumour-infiltrating B cells in human cancer: a new force in immunotherapy. Biomark. Res. 11, 28 (2023).
Google Scholar
Chen, P., Chu, Y. & Liu, R. Tumour-reactive plasma cells in antitumour immunity: current insights and future prospects. Immunother. Adv. 4, ltae003 (2024).
Google Scholar
Singh, R., Kim, Y.-H., Lee, S.-J., Eom, H.-S. & Choi, B. K. 4-1BB immunotherapy: advances and hurdles. Exp. Mol. Med. 56, 32–39 (2024).
Google Scholar
Wolf, N. K., Kissiov, D. U. & Raulet, D. H. Roles of natural killer cells in immunity to cancer, and applications to immunotherapy. Nat. Rev. Immunol. 23, 90–105 (2023).
Google Scholar
Hazeldine, J. & Lord, J. M. The impact of ageing on natural killer cell function and potential consequences for health in older adults. Ageing Res. Rev. 12, 1069–1078 (2013).
Google Scholar
Jin, S. et al. Inference and analysis of cell-cell communication using CellChat. Nat. Commun. 12, 1088 (2021).
Google Scholar
Böttcher, J. P. et al. NK cells stimulate recruitment of cDC1 into the tumor microenvironment promoting cancer immune control. Cell 172, 1022–1037.e14 (2018).
Google Scholar
Guimond, M. et al. In vivo role of Flt3 ligand and dendritic cells in NK cell homeostasis. J. Immunol. 184, 2769–2775 (2010).
Google Scholar
van Vlerken-Ysla, L., Tyurina, Y. Y., Kagan, V. E. & Gabrilovich, D. I. Functional states of myeloid cells in cancer. Cancer Cell 41, 490–504 (2023).
Google Scholar
Jackaman, C. et al. Aging and cancer: the role of macrophages and neutrophils. Ageing Res. Rev. 36, 105–116 (2017).
Google Scholar
Jackaman, C. & Nelson, D. J. Are macrophages, myeloid derived suppressor cells and neutrophils mediators of local suppression in healthy and cancerous tissues in aging hosts? Exp. Gerontol. 54, 53–57 (2014).
Google Scholar
Li, Y. et al. Age-related macrophage alterations are associated with carcinogenesis of colorectal cancer. Carcinogenesis 43, 1039–1049 (2022).
Google Scholar
Alicea, G. M. et al. Changes in aged fibroblast lipid metabolism induce age-dependent melanoma cell resistance to targeted therapy via the fatty acid transporter FATP2. Cancer Discov. 10, 1282–1295 (2020).
Google Scholar
Hurez, V. et al. Mitigating age-related immune dysfunction heightens the efficacy of tumor immunotherapy in aged mice. Cancer Res. 72, 2089–2099 (2012).
Google Scholar
Prieto, L. I. et al. Senescent alveolar macrophages promote early-stage lung tumorigenesis. Cancer Cell 41, 1261–1275.e6 (2023).
Google Scholar
Duan, R. et al. Aging-induced immune microenvironment remodeling fosters melanoma in male mice via γδ17-neutrophil-CD8 axis. Nat. Commun. 15, 10860 (2024). This study revealed that, in aged male mice, IL-17+ γδ T cells recruit neutrophils to the TME where they suppress CD8+ T cell effector function, resulting in enhanced melanoma, highlighting an age-associated and sex-associated immunosuppressive axis.
Google Scholar
Kumar, S. et al. Uncovering therapeutic targets for macrophage-mediated T cell suppression and PD-L1 therapy sensitization. Cell Rep. Med. 5, 101698 (2024).
Google Scholar
Coussens, L. M., Zitvogel, L. & Palucka, A. K. Neutralizing tumor-promoting chronic inflammation: a magic bullet? Science 339, 286–291 (2013).
Google Scholar
Barry, S. T., Gabrilovich, D. I., Sansom, O. J., Campbell, A. D. & Morton, J. P. Therapeutic targeting of tumour myeloid cells. Nat. Rev. Cancer 23, 216–237 (2023).
Google Scholar
Lue, J. C. & Radisky, D. C. From embryogenesis to senescence: the role of mammary gland physiology in breast cancer risk. Cancers 17, 787 (2025).
Google Scholar
Khodr, Z. G. et al. Circulating sex hormones and terminal duct lobular unit involution of the normal breast. Cancer Epidemiol. Biomark. Prev. 23, 2765–2773 (2014).
Google Scholar
Zirbes, A. et al. Changes in immune cell types with age in breast are consistent with a decline in immune surveillance and increased immunosuppression. J. Mammary Gland. Biol. Neoplasia 26, 247–261 (2021). This study characterized age-related changes in immune cell composition and localization within normal human breast tissue, revealing a decline in peri-epithelial T cells and B cells and increased immunosuppressive macrophages with age, suggesting that age fosters immunosenescence and inflammation, increasing the susceptibility to breast cancer.
Google Scholar
Shalabi, S. F. et al. Evidence for accelerated aging in mammary epithelia of women carrying germline BRCA1 or BRCA2 mutations. Nat. Aging 1, 838–849 (2021).
Google Scholar
Sayaman, R. W. et al. Luminal epithelial cells integrate variable responses to aging into stereotypical changes that underlie breast cancer susceptibility. eLife 13, e95720 (2024).
Google Scholar
Yan, P. et al. Midkine as a driver of age-related changes and increase in mammary tumorigenesis. Cancer Cell 42, 1936–1954.e9 (2024). This study identified a role for midkine in driving ageing-related changes in the mammary gland that associate with a reduction in TILs and promote breast cancer development.
Google Scholar
Catena, X. et al. Systemic rewiring of dendritic cells by melanoma-secreted midkine impairs immune surveillance and response to immune checkpoint blockade. Nat. Cancer 6, 682–701 (2025).
Google Scholar
Cerezo-Wallis, D. et al. Midkine rewires the melanoma microenvironment toward a tolerogenic and immune-resistant state. Nat. Med. 26, 1865–1877 (2020).
Google Scholar
Harper, E. I. & Weeraratna, A. T. A wrinkle in TIME: how changes in the aging ECM drive the remodeling of the tumor immune microenvironment. Cancer Discov. 13, 1973–1981 (2023).
Google Scholar
Du, H. et al. Tuning immunity through tissue mechanotransduction. Nat. Rev. Immunol. 23, 174–188 (2023).
Google Scholar
Kaur, A. et al. Remodeling of the collagen matrix in aging skin promotes melanoma metastasis and affects immune cell motility. Cancer Discov. 9, 64–81 (2019).
Google Scholar
Marino, G. E. & Weeraratna, A. T. A glitch in the matrix: age-dependent changes in the extracellular matrix facilitate common sites of metastasis. Aging Cancer 1, 19–29 (2020).
Google Scholar
Pettan-Brewer, C. et al. B16 melanoma tumor growth is delayed in mice in an age-dependent manner. Pathobiol. Aging Age Relat. Dis. 2, 19182 (2012).
Reed, M. J. et al. The effects of aging on tumor growth and angiogenesis are tumor-cell dependent. Int. J. Cancer 120, 753–760 (2007).
Google Scholar
Klement, H. et al. Atherosclerosis and vascular aging as modifiers of tumor progression, angiogenesis, and responsiveness to therapy. Am. J. Pathol. 171, 1342–1351 (2007).
Google Scholar
Marinho, A., Soares, R., Ferro, J., Lacerda, M. & Schmitt, F. C. Angiogenesis in breast cancer is related to age but not to other prognostic parameters. Pathol. Res. Pract. 193, 267–273 (1997).
Google Scholar
Khan, K. A. & Kerbel, R. S. Improving immunotherapy outcomes with anti-angiogenic treatments and vice versa. Nat. Rev. Clin. Oncol. 15, 310–324 (2018).
Google Scholar
Donato, A. J., Morgan, R. G., Walker, A. E. & Lesniewski, L. A. Cellular and molecular biology of aging endothelial cells. J. Mol. Cell. Cardiol. 89, 122–135 (2015).
Google Scholar
Liu, S. et al. ROS fine-tunes the function and fate of immune cells. Int. Immunopharmacol. 119, 110069 (2023).
Google Scholar
Marino-Bravante, G. E. et al. Age-dependent loss of HAPLN1 erodes vascular integrity via indirect upregulation of endothelial ICAM1 in melanoma. Nat. Aging 4, 350–363 (2024).
Google Scholar
Bui, T. M., Wiesolek, H. L. & Sumagin, R. ICAM-1: a master regulator of cellular responses in inflammation, injury resolution, and tumorigenesis. J. Leukoc. Biol. 108, 787–799 (2020).
Google Scholar
Upadhaya, S., Neftelinov, S. T., Hodge, J. & Campbell, J. Challenges and opportunities in the PD1/PDL1 inhibitor clinical trial landscape. Nat. Rev. Drug Discov. 21, 482–483 (2022).
Google Scholar
Karin, O., Agrawal, A., Porat, Z., Krizhanovsky, V. & Alon, U. Senescent cell turnover slows with age providing an explanation for the Gompertz law. Nat. Commun. 10, 5495 (2019).
Google Scholar
Coppé, J.-P., Desprez, P.-Y., Krtolica, A. & Campisi, J. The senescence-associated secretory phenotype: the dark side of tumor suppression. Annu. Rev. Pathol. 5, 99–118 (2010).
Google Scholar
Zhou, L., Ma, B. & Ruscetti, M. Cellular senescence offers distinct immunological vulnerabilities in cancer. Trends Cancer 11, 334–350 (2024).
Google Scholar
Faget, D. V., Ren, Q. & Stewart, S. A. Unmasking senescence: context-dependent effects of SASP in cancer. Nat. Rev. Cancer 19, 439–453 (2019).
Google Scholar
Ruhland, M. K. et al. Stromal senescence establishes an immunosuppressive microenvironment that drives tumorigenesis. Nat. Commun. 7, 11762 (2016).
Google Scholar
Feig, C. et al. Targeting CXCL12 from FAP-expressing carcinoma-associated fibroblasts synergizes with anti-PD-L1 immunotherapy in pancreatic cancer. Proc. Natl Acad. Sci. USA 110, 20212–20217 (2013).
Google Scholar
Meguro, S. et al. Preexisting senescent fibroblasts in the aged bladder create a tumor-permissive niche through CXCL12 secretion. Nat. Aging 4, 1582–1597 (2024).
Google Scholar
Assouline, B. et al. Senescent cancer-associated fibroblasts in pancreatic adenocarcinoma restrict CD8+ T cell activation and limit responsiveness to immunotherapy in mice. Nat. Commun. 15, 6162 (2024).
Google Scholar
Ye, J. et al. Senescent CAFs mediate immunosuppression and drive breast cancer progression. Cancer Discov. 14, 1302–1323 (2024). This study, together with Belle et al. (2024), identified a role for a population of senescent myofibroblastic CAFs in facilitating immune suppression in the TME by limiting NK cell-mediated anti-cancer immunity in a preclinical breast cancer model with parallel phenotypes in human cancer.
Google Scholar
Belle, J. I. et al. Senescence defines a distinct subset of myofibroblasts that orchestrates immunosuppression in pancreatic cancer. Cancer Discov. 14, 1324–1355 (2024).
Google Scholar
Pereira, B. I. et al. Senescent cells evade immune clearance via HLA-E-mediated NK and CD8+ T cell inhibition. Nat. Commun. 10, 2387 (2019).
Google Scholar
Fane, M. & Weeraratna, A. T. How the ageing microenvironment influences tumour progression. Nat. Rev. Cancer 20, 89–106 (2020).
Google Scholar
Ye, J., Melam, A. & Stewart, S. A. Stromal senescence contributes to age-related increases in cancer. Nat. Rev. Cancer (2025).
Google Scholar
Kaur, A. et al. sFRP2 in the aged microenvironment drives melanoma metastasis and therapy resistance. Nature 532, 250–254 (2016).
Google Scholar
Fane, M. E. et al. Stromal changes in the aged lung induce an emergence from melanoma dormancy. Nature 606, 396–405 (2022).
Google Scholar
Zabransky, D. J. et al. Fibroblasts in the aged pancreas drive pancreatic cancer progression. Cancer Res. 84, 1221–1236 (2024). Using proteomics, the authors demonstrated that ageing alters pancreatic fibroblast secretomes, notably increasing GDF15 production, which promotes tumour progression via AKT activation in aged mice, revealing age-dependent microenvironmental mechanisms driving pancreatic cancer progression and potential therapeutic vulnerabilities.
Google Scholar
Ratnam, N. M. et al. NF-κB regulates GDF-15 to suppress macrophage surveillance during early tumor development. J. Clin. Invest. 127, 3796–3809 (2017).
Google Scholar
Carlson, E. G. et al. CD105+ fibroblasts support an immunosuppressive niche in women at high risk of breast cancer initiation. Breast Cancer Res. 27, 81 (2025).
Google Scholar
Ahmed, B. & Si, H. The aging of adipocytes increases expression of pro-inflammatory cytokines chronologically. Metabolites 11, 292 (2021).
Google Scholar
Nguyen, T. T. & Corvera, S. Adipose tissue as a linchpin of organismal ageing. Nat. Metab. 6, 793–807 (2024).
Google Scholar
Tanaka, T., Narazaki, M. & Kishimoto, T. IL-6 in inflammation, immunity, and disease. Cold Spring Harb. Perspect. Biol. 6, a016295 (2014).
Google Scholar
Yoshimura, T. et al. Non-myeloid cells are major contributors to innate immune responses via production of monocyte chemoattractant protein-1/CCL2. Front. Immunol. 4, 482 (2014).
Google Scholar
Chen, A. Y., Wolchok, J. D. & Bass, A. R. TNF in the era of immune checkpoint inhibitors: friend or foe? Nat. Rev. Rheumatol. 17, 213–223 (2021).
Google Scholar
Gurung, S. et al. Stromal lipid species dictate melanoma metastasis and tropism. Cancer Cell 43, 1108–1124.e11 (2025).
Google Scholar
Hubler, M. J. & Kennedy, A. J. Role of lipids in the metabolism and activation of immune cells. J. Nutr. Biochem. 34, 1–7 (2016).
Google Scholar
Lazure, F. & Gomes, A. P. Cancer progression through the lens of age-induced metabolic reprogramming. Nat. Rev. Cancer (2025).
Google Scholar
Yaniv, D., Mattson, B., Talbot, S., Gleber-Netto, F. O. & Amit, M. Targeting the peripheral neural-tumour microenvironment for cancer therapy. Nat. Rev. Drug Discov. 23, 780–796 (2024).
Google Scholar
White, C. W., Xie, J. H. & Ventura, S. Age-related changes in the innervation of the prostate gland: implications for prostate cancer initiation and progression. Organogenesis 9, 206–215 (2013).
Google Scholar
Ayala, G. E. et al. Cancer-related axonogenesis and neurogenesis in prostate cancer. Clin. Cancer Res. 14, 7593–7603 (2008).
Google Scholar
Al-Danakh, A. et al. Aging-related biomarker discovery in the era of immune checkpoint inhibitors for cancer patients. Front. Immunol. 15, 1348189 (2024).
Google Scholar
Voruganti, T., Soulos, P. R., Mamtani, R., Presley, C. J. & Gross, C. P. Association between age and survival trends in advanced non-small cell lung cancer after adoption of immunotherapy. JAMA Oncol. 9, 334–341 (2023).
Google Scholar
Yin, J. et al. The efficacy of immune checkpoint inhibitors is limited in elderly NSCLC: a retrospective efficacy study and meta-analysis. Aging 15, 15025–15049 (2023).
Google Scholar
Ding, Y. et al. Age-related efficacy of immunotherapies in advanced non-small cell lung cancer: a comprehensive meta-analysis. Lung Cancer 195, 107925 (2024).
Google Scholar
Ibrahim, T., Mateus, C., Baz, M. & Robert, C. Older melanoma patients aged 75 and above retain responsiveness to anti-PD1 therapy: results of a retrospective single-institution cohort study. Cancer Immunol. Immunother. 67, 1571–1578 (2018).
Google Scholar
Li, P. et al. The impact of immunosenescence on the efficacy of immune checkpoint inhibitors in melanoma patients: a meta-analysis. Onco. Targets Ther. 11, 7521–7527 (2018).
Google Scholar
Woo, T. E. et al. Effectiveness of immune checkpoint inhibitor with anti-PD-1 monotherapy or in combination with ipilimumab in younger versus older adults with advanced melanoma. Curr. Oncol. 30, 8936–8947 (2023).
Google Scholar
Kim, C. M. et al. The efficacy of immune checkpoint inhibitors in elderly patients: a meta-analysis and meta-regression. ESMO Open 7, 100577 (2022).
Google Scholar
Le, D. T. et al. PD-1 blockade in tumors with mismatch-repair deficiency. N. Engl. J. Med. 372, 2509–2520 (2015).
Google Scholar
Overman, M. J. et al. Nivolumab plus relatlimab in patients with previously treated microsatellite instability-high/mismatch repair-deficient metastatic colorectal cancer: the phase II CheckMate 142 study. J. Immunother. Cancer 12, e008689 (2024).
Google Scholar
André, T. et al. Pembrolizumab in microsatellite-instability-high advanced colorectal cancer. N. Engl. J. Med. 383, 2207–2218 (2020).
Google Scholar
Elias, R. et al. Efficacy of PD-1 & PD-L1 inhibitors in older adults: a meta-analysis. J. Immunother. Cancer 6, 26 (2018).
Google Scholar
Nishijima, T. F., Muss, H. B., Shachar, S. S. & Moschos, S. J. Comparison of efficacy of immune checkpoint inhibitors (ICIs) between younger and older patients: a systematic review and meta-analysis. Cancer Treat. Rev. 45, 30–37 (2016).
Google Scholar
Cil, E. & Gomes, F. Toxicity of cancer immunotherapies in older patients: does age make a difference? Drugs Aging 41, 787–794 (2024).
Google Scholar
Cook, S. L. et al. Immune checkpoint inhibitors in geriatric oncology. Curr. Oncol. Rep. 26, 562–572 (2024).
Google Scholar
Spigel, D. R. et al. Safety, efficacy, and patient-reported health-related quality of life and symptom burden with nivolumab in patients with advanced non-small cell lung cancer, including patients aged 70 years or older or with poor performance status (CheckMate 153). J. Thorac. Oncol. 14, 1628–1639 (2019).
Google Scholar
Felip, E. et al. CheckMate 171: a phase 2 trial of nivolumab in patients with previously treated advanced squamous non-small cell lung cancer, including ECOG PS 2 and elderly populations. Eur. J. Cancer 127, 160–172 (2020).
Google Scholar
US National Library of Medicine. Clinicaltrials.gov (2019).
US National Library of Medicine. Clinicaltrials.gov (2023).
US National Library of Medicine. Clinicaltrials.gov (2024).
US National Library of Medicine. Clinicaltrials.gov (2023).
US National Library of Medicine. Clinicaltrials.gov (2018).
US National Library of Medicine. Clinicaltrials.gov (2023).
US National Library of Medicine. Clinicaltrials.gov (2024).
US National Library of Medicine. Clinicaltrials.gov (2023).
Johnson, D. B., Sullivan, R. J. & Menzies, A. M. Immune checkpoint inhibitors in challenging populations. Cancer 123, 1904–1911 (2017).
Google Scholar
Blanco, R. et al. Pembrolizumab as first-line treatment for advanced NSCLC in older adults: a phase II clinical trial evaluating geriatric and quality-of-life outcomes. Lung Cancer 183, 107318 (2023).
Google Scholar
Tran Van Hoi, E. et al. Blood based immune biomarkers associated with clinical frailty scale in older patients with melanoma receiving checkpoint inhibitor immunotherapy. Immun. Ageing 21, 83 (2024). This is the first prospective clinical trial to use both frailty assessment and immunophenotyping to determine whether advanced age and frailty correlate with baseline immune health and responses to anti-PD1-checkpoint blockade therapy.
Google Scholar
Bruijnen, C. P. et al. Frailty and checkpoint inhibitor toxicity in older patients with melanoma. Cancer 128, 2746–2752 (2022).
Google Scholar
La, J. et al. Real-world outcomes for patients treated with immune checkpoint inhibitors in the Veterans Affairs system. JCO Clin. Cancer Inform. 4, 918–928 (2020).
Google Scholar
US National Library of Medicine. Clinicaltrials.gov (2017).
US National Library of Medicine. Clinicaltrials.gov (2020).
Reitsema, R. D., Kumawat, A. K., Hesselink, B.-C., van Baarle, D. & van Sleen, Y. Effects of ageing and frailty on circulating monocyte and dendritic cell subsets. NPJ Aging 10, 17 (2024).
Google Scholar
Samson, L. D. et al. In-depth immune cellular profiling reveals sex-specific associations with frailty. Immun. Ageing 17, 20 (2020).
Google Scholar
Sayed, N. et al. An inflammatory aging clock (iAge) based on deep learning tracks multimorbidity, immunosenescence, frailty and cardiovascular aging. Nat. Aging 1, 598–615 (2021).
Google Scholar
Nakajima, Y., Chamoto, K., Oura, T. & Honjo, T. Critical role of the CD44lowCD62Llow CD8+ T cell subset in restoring antitumor immunity in aged mice. Proc. Natl Acad. Sci. USA 118, e2103730118 (2021).
Google Scholar
Padrón, Á. et al. Age effects of distinct immune checkpoint blockade treatments in a mouse melanoma model. Exp. Gerontol. 105, 146–154 (2018).
Google Scholar
Garcia, M. G. et al. Immune checkpoint expression and relationships to anti-PD-L1 immune checkpoint blockade cancer immunotherapy efficacy in aged versus young mice. Aging Cancer 3, 68–83 (2022).
Google Scholar
Sekido, K. et al. Alterations in composition of immune cells and impairment of anti-tumor immune response in aged oral cancer-bearing mice. Oral. Oncol. 99, 104462 (2019).
Google Scholar
Ladomersky, E. et al. Advanced age increases immunosuppression in the brain and decreases immunotherapeutic efficacy in subjects with glioblastoma. Clin. Cancer Res. 26, 5232–5245 (2020).
Google Scholar
Mo, D.-C. et al. The role of PD-L1 in patients with non-small cell lung cancer receiving neoadjuvant immune checkpoint inhibitor plus chemotherapy: a meta-analysis. Sci. Rep. 14, 26200 (2024).
Google Scholar
Cortes, J. et al. Contribution of tumour and immune cells to PD-L1 expression as a predictive biomarker in metastatic triple-negative breast cancer: exploratory analysis from KEYNOTE-119. J. Pathol. Clin. Res. 10, e12371 (2024).
Google Scholar
Schoenfeld, A. J. et al. Clinical and molecular correlates of PD-L1 expression in patients with lung adenocarcinomas. Ann. Oncol. 31, 599–608 (2020).
Google Scholar
Mirza, N. et al. B7-H1 expression on old CD8+ T cells negatively regulates the activation of immune responses in aged animals. J. Immunol. 184, 5466–5474 (2010). This was the first preclinical study to assess the efficacy of PDL1-checkpoint blockade in aged versus young adult mice; they found that aged mice upregulate PDL1, rendering checkpoint blockade highly effective.
Google Scholar
Sun, X. et al. Longitudinal analysis reveals age-related changes in the T cell receptor repertoire of human T cell subsets. J. Clin. Invest. 132, e158122 (2022).
Google Scholar
Ladomersky, E. et al. Advanced age negatively impacts survival in an experimental brain tumor model. Neurosci. Lett. 630, 203–208 (2016).
Google Scholar
Gardner, J. K., Jackaman, C., Mamotte, C. D. S. & Nelson, D. J. The regulatory status adopted by lymph node dendritic cells and T cells during healthy aging is maintained during cancer and may contribute to reduced responses to immunotherapy. Front. Med. 5, 337 (2018).
Freedman, R. A. et al. “ADVANCE” (a pilot trial) ADjuVANt chemotherapy in the elderly: developing and evaluating lower-toxicity chemotherapy options for older patients with breast cancer. J. Geriatr. Oncol. 14, 101377 (2023). This pragmatic pilot trial evaluated the feasibility of two neoadjuvant or adjuvant chemotherapy regimens in adults over 70 years of age with HER2-negative breast cancer and found that neither regimen met pre-defined feasibility thresholds, underscoring the need for more tolerable, age-adapted therapeutic strategies for older patients, who are underrepresented in clinical trials.
Google Scholar
Piccart, M. et al. 70-gene signature as an aid for treatment decisions in early breast cancer: updated results of the phase 3 randomised MINDACT trial with an exploratory analysis by age. Lancet Oncol. 22, 476–488 (2021).
Google Scholar
Guida, J. L., Gallicchio, L. & Green, P. A. Are early-onset cancers an example of accelerated biological aging? JAMA Oncol. 11, 690–691 (2025).
Google Scholar
Castaño, Z., Tracy, K. & McAllister, S. S. The tumor macroenvironment and systemic regulation of breast cancer progression. Int. J. Dev. Biol. 55, 889–897 (2011).
Google Scholar
Duan, R., Fu, Q., Sun, Y. & Li, Q. Epigenetic clock: a promising biomarker and practical tool in aging. Ageing Res. Rev. 81, 101743 (2022).
Google Scholar
Yamamoto, R. et al. Tissue-specific impacts of aging and genetics on gene expression patterns in humans. Nat. Commun. 13, 5803 (2022).
Google Scholar
Slieker, R. C., Relton, C. L., Gaunt, T. R., Slagboom, P. E. & Heijmans, B. T. Age-related DNA methylation changes are tissue-specific with ELOVL2 promoter methylation as exception. Epigenetics Chromatin 11, 25 (2018).
Google Scholar
Dugué, P.-A. et al. Biological aging measures based on blood DNA methylation and risk of cancer: a prospective study. JNCI Cancer Spectr. 5, kaa109 (2021).
Tserel, L. et al. Age-related profiling of DNA methylation in CD8+ T cells reveals changes in immune response and transcriptional regulator genes. Sci. Rep. 5, 13107 (2015).
Google Scholar
Tsukamoto, H. et al. Aging-associated and CD4 T-cell-dependent ectopic CXCL13 activation predisposes to anti-PD-1 therapy-induced adverse events. Proc. Natl Acad. Sci. USA 119, e2205378119 (2022).
Google Scholar
Weyh, C., Krüger, K. & Strasser, B. Physical activity and diet shape the immune system during aging. Nutrients 12, 622 (2020).
Google Scholar
Bachmann, M. C. et al. The challenge by multiple environmental and biological factors induce inflammation in aging: their role in the promotion of chronic disease. Front. Immunol. 11, 570083 (2020).
Google Scholar
Besedovsky, L., Lange, T. & Born, J. Sleep and immune function. Pflug. Arch. 463, 121–137 (2012).
Google Scholar
Dhabhar, F. S. Effects of stress on immune function: the good, the bad, and the beautiful. Immunol. Res. 58, 193–210 (2014).
Google Scholar
Walford, R. L. The immunologic theory of aging. Gerontologist 4, 195–197 (1964).
Google Scholar
Henson, S. M. et al. p38 signaling inhibits mTORC1-independent autophagy in senescent human CD8+ T cells. J. Clin. Invest. 124, 4004–4016 (2014).
Google Scholar
Simon, S. & Labarriere, N. PD-1 expression on tumor-specific T cells: friend or foe for immunotherapy? Oncoimmunology 7, e1364828 (2017).
Google Scholar
Jenkins, E., Whitehead, T., Fellermeyer, M., Davis, S. J. & Sharma, S. The current state and future of T-cell exhaustion research. Oxf. Open Immunol. 4, iqad006 (2023).
Google Scholar
Akbar, A. N. & Henson, S. M. Are senescence and exhaustion intertwined or unrelated processes that compromise immunity? Nat. Rev. Immunol. 11, 289–295 (2011).
Google Scholar
Yang, Y., Li, T. & Nielsen, M. E. Aging and cancer mortality: dynamics of change and sex differences. Exp. Gerontol. 47, 695–705 (2012).
Google Scholar
Bonafè, M. et al. Inflamm-aging: why older men are the most susceptible to SARS-CoV-2 complicated outcomes. Cytokine Growth Factor Rev. 53, 33–37 (2020).
Google Scholar
Sefik, E. et al. Inflammasome activation in infected macrophages drives COVID-19 pathology. Nature 606, 585–593 (2022).
Google Scholar
Ravichandran, S. et al. Distinct baseline immune characteristics associated with responses to conjugated and unconjugated pneumococcal polysaccharide vaccines in older adults. Nat. Immunol. 25, 316–329 (2024).
Google Scholar
Pido-Lopez, J., Imami, N. & Aspinall, R. Both age and gender affect thymic output: more recent thymic migrants in females than males as they age. Clin. Exp. Immunol. 125, 409–413 (2001).
Google Scholar
Castro, A. et al. Strength of immune selection in tumors varies with sex and age. Nat. Commun. 11, 4128 (2020). This study demonstrated that the strength of MHC-mediated immune selection during tumorigenesis varies by age and sex, with younger and female patients experiencing poorer response rates to ICI therapy than those of older and male patients due to reduced neoantigen availability.
Google Scholar
Xiao, T. et al. Hallmarks of sex bias in immuno-oncology: mechanisms and therapeutic implications. Nat. Rev. Cancer 24, 338–355 (2024).
Google Scholar
Thompson, D. J. et al. Genetic predisposition to mosaic Y chromosome loss in blood. Nature 575, 652–657 (2019).
Google Scholar
Grigoryan, A. et al. Attrition of X chromosome inactivation in aged hematopoietic stem cells. Stem Cell Rep. 16, 708–716 (2021).
Google Scholar
Forsberg, L. A. et al. Mosaic loss of chromosome Y in peripheral blood is associated with shorter survival and higher risk of cancer. Nat. Genet. 46, 624–628 (2014).
Google Scholar
Chhabra, Y. et al. Sex-dependent effects in the aged melanoma tumor microenvironment influence invasion and resistance to targeted therapy. Cell 187, 6016–6034.e25 (2024).
Google Scholar
Warde, K. M. et al. Senescence-induced immune remodeling facilitates metastatic adrenal cancer in a sex-dimorphic manner. Nat. Aging 3, 846–865 (2023).
Google Scholar
link