NMR metabolomic signatures of healthy lifestyle and incident MASLD

Baseline characteristics of study participants
The study cohort included 179,261 UK Biobank participants, of whom 2,422 (1.35%) developed incident MASLD during follow-up. Participants who subsequently developed MASLD exhibited significantly higher BMI (31.16 ± 5.53 vs. 27.33 ± 4.61 kg/m2, P < 0.001), with 52.97% being obese compared to 23.23% in controls. They demonstrated lower socioeconomic status, including reduced university education (25.52% vs. 35.65%) and higher rates of low income (29.31% vs. 20.44%). Additionally, the MASLD group showed greater baseline comorbidity burden, with higher prevalences of diabetes mellitus (16.47% vs. 4.80%), hypertension (50.12% vs. 29.48%), and CVD (14.91% vs. 7.37%, all P < 0.001). Healthy lifestyle adherence was also significantly lower in those who developed MASLD (Table 1).
Identification of metabolic signatures for lifestyle
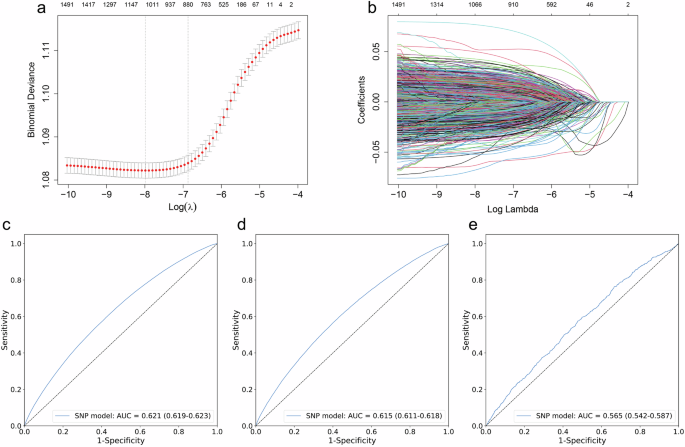
Using elastic network regularized regression analysis, we successfully identified a 94-metabolite signature that reflected comprehensive metabolic responses to healthy lifestyle behaviors (Fig. 1, sFig. 2). The metabolic signature spanned diverse biochemical pathways, with relative lipoprotein lipid concentrations constituting the largest component (37.23%, n = 35), followed by lipoprotein subclasses (24.47%, n = 23). Amino acids and fatty acids each represented 10.64% (n = 10) of the signature, while glycolysis-related metabolites comprised 4.26% (n = 4) (sFig. 3). Additional components included ketone bodies (3.19%, n = 3), fluid balance markers (2.13%, n = 2), lipoprotein particle sizes (2.13%, n = 2), and other lipids (2.13%, n = 2), with single representatives from apolipoproteins, inflammation markers, and total lipids (1.06% each, n = 1).
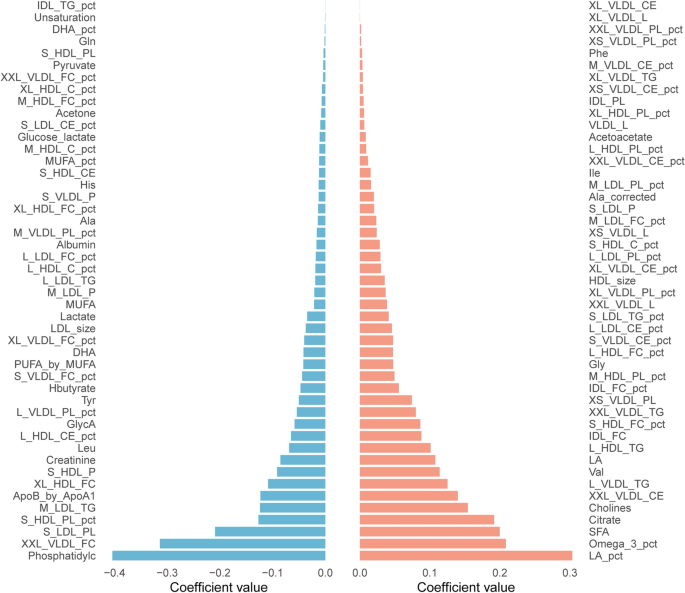
Metabolites ranked from the highest to the lowest elastic network positive and negative regression coefficients for lifestyle.
The metabolic signature demonstrated distinctive directional relationships with healthy lifestyle adherence (Fig. 1, sTable 3). Metabolites showing the strongest positive associations with healthy lifestyle included LA_pct, Omega_3_pct, SFA, Citrate, and, Cholines. Conversely, metabolites exhibiting the most pronounced negative correlations encompassed Phosphatidylc, XXL_VLDL_FC, S_LDL_PL, S_HDL_PL_pct, and M_LDL_TG. Correlation analyses revealed robust associations between the 94-metabolite signature and both the composite lifestyle score and individual lifestyle components (smoking, alcohol, physical activity, DASH diet), as illustrated in sFig. 4. Baseline metabolite concentrations stratified by MASLD development status are presented in sTable 4.
Associations of lifestyle and the related metabolic profiles with MASLD
Strong protective associations between healthy lifestyle, related metabolic profiles, and MASLD incidence were demonstrated in Table 2. In the fully adjusted Model 3, each 1 factor increment in the lifestyle score and 1 unit increment in the metabolic signature corresponded to 14.8% (HR = 0.852, 95% CI 0.820–0.885) and 65.9% (HR = 0.341, 95% CI 0.311–0.373) reduced risk of MASLD, respectively. When participants were categorized into tertiles, those in the highest versus lowest tertile of lifestyle scores and metabolic signatures exhibited 33.2% (HR = 0.668, 95% CI 0.571–0.782) and 74.3% (HR = 0.257, 95% CI 0.220–0.301) lower MASLD risk. RCS analyses revealed linear dose–response relationships for both lifestyle scores (P-nonlinear = 0.727) and metabolic signatures (P-nonlinear = 0.105) (Fig. 2). The single healthy lifestyle factor, including smoking, physical activity and the DASH diet standard also was associated with a reduced risk of deeloping MASLD (sTable 5).
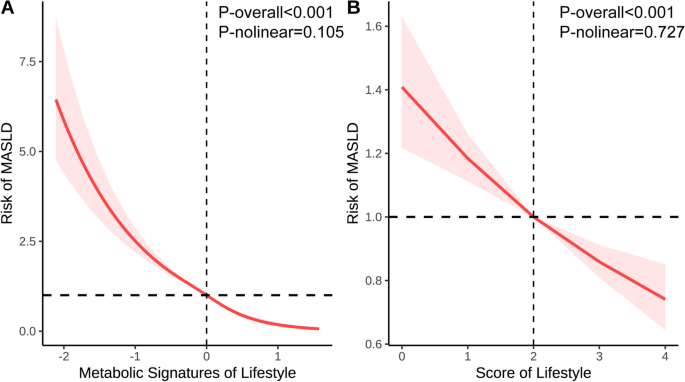
RCS analysis of the associations of lifestyle score and the related metabolic profiles with MASLD. Models were adjusted for age, sex, race, CVD, and cancer. MASLD: Metabolic dysfunction-associated steatotic liver disease; CVD: Cardiovascular disease.
Individual metabolite analyses (sTable 6) revealed specific biomarkers underlying the protective associations. Notable risk-reducing metabolites included XL_VLDL_CE_pct (HR = 0.523, 95% CI 0.494–0.554), PUFA_by_MUFA (HR = 0.525, 95% CI 0.503–0.548), LA_pct (HR = 0.573, 95% CI 0.552–0.596), various HDL cholesterol percentages, and so on. Conversely, several metabolites showed positive associations with MASLD risk, including L_HDL_PL_pct(HR = 1.812, 95% CI 1.703–1.927), MUFA_pct(HR = 1.727, 95% CI 1.665–1.792), M_HDL_PL_pct(HR = 1.678, 95% CI 1.620–1.737), L_VLDL_PL_pct(HR = 1.567, 95% CI 1.523–1.612), various VLDL components, and branched-chain amino acids.
Subgroup analyses (Fig. 3, sTable 7) revealed consistent protective associations across diverse population strata. Sex significantly modified the metabolite profiles -MASLD association (P-interaction = 0.009), with stronger protective effects observed in Female (HR = 0.298, 95% CI 0.259–0.344) compared to Male (HR = 0.375, 95% CI 0.331–0.425). History of CVD significantly influenced associations of metabolic signature with MASLD risk (P-interaction = 0.001), showing attenuated protective effects in participants with pre-existing CVD (HR = 0.492, 95% CI 0.38–0.636) when compared to without CVD (HR = 0.322, 95% CI 0.293–0.354). The metabolic signature maintained robust and consistent associations across other subgroups.
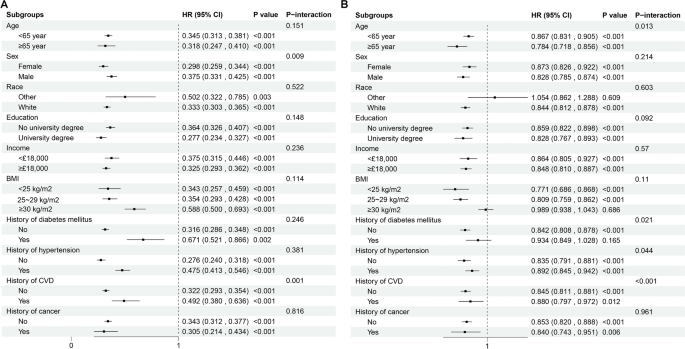
Subgroup of the associations of lifestyle score and the related metabolic profiles with MASLD. (A) Subgroup of the associations of metabolic profiles with MASLD; (B) Subgroup of the associations of lifestyle score with MASLD. Models were adjusted for age, sex, race, education, income, CVD, and cancer. MASLD: Metabolic dysfunction-associated steatotic liver disease; CVD: Cardiovascular disease.
Mediation of metabolic signature on the association of lifestyle with MASLD
Causal mediation analysis demonstrated that metabolic signatures substantially mediated the protective association between healthy lifestyle behaviors and MASLD risk (Table 3, sTable 8). The 94-metabolite signature served as a crucial mediator in the lifestyle-MASLD pathway, accounting for 55.80% (95% CI 47.85–85.28%) of the total protective association between lifestyle score and MASLD risk. Among individual lifestyle components, Smoking cessation and DASH diet adherence showed the strong mediation effect, with metabolic alterations explaining 37.32% and 36.98% of their protective association with MASLD risk, respectively. While physical activity exhibited a more modest but significant mediation effect of 12.48% .Addtionally, the Evalue value of total effect, direct effect, and indirect effect were all relatively high, which implied the mediation effect was robust (sTable 9). The parallel mediation analysis showed that the total mediating effect of metabolic signatures, BMI, diabetes and hypertension in the relationship between lifestyle and MASLD was as high as 86.21%.
Individual metabolite mediation analysis (sTable 10) identified specific biomarkers contributing most prominently to the overall mediation effect. Fatty acid metabolism emerged as the most influential mediator, with PUFA_by_MUFA contributing 52.62% mediation, followed by LA_pct at 51.75%. Lipoprotein metabolism markers played substantial mediating roles, with various cholesterol ester percentages contributing between 15 and 25% mediation. Additional important mediators included triglyceride-related metabolites, with M_LDL_TG contributing 18.69% and various VLDL triglyceride components mediating 5–25% of the association. These findings highlight the multi-pathway nature of lifestyle-mediated metabolic protection against MASLD development.
Sensitive analysis
Comprehensive sensitivity analyses confirmed the robustness of our findings across different analytical strategies. After excluding participants with missing covariates (n = 159,429), the metabolic signature maintained strong protective associations with MASLD (HR: 0.341, 95% CI 0.311–0.373) with mediation effects of 49.54% (sTables 10, 11). Excluding MASLD cases within two years of follow-up (n = 179,181) preserved protective associations (HR: 0.338, 95% CI 0.308–0.371) with increased mediation proportions of 58.43% (sTables 12, 13). When restricting to participants without baseline cardiovascular disease (n = 165,859), associations were slightly strengthened (HR: 0.329, 95% CI 0.301–0.360) with mediation effects reaching 61.68% (sTables 14, 15). RCS analyses consistently demonstrated linear dose–response relationships across all sensitivity analyses (sFigs. 5–7).
link